News & Views
Read the latest news from Gloucestershire Health and Care NHS Foundation Trust

Developing a Vocational Rehabilitation Service
Our Occupational Therapy Service and QI (Quality Improvement) team has supported Rosebank Primary...

Supporting our Community Hospital Gardens
The green spaces at three of our community hospital sites are supported by contractors Cotswold...

Celebrating 150 years of Stroud General Hospital
To mark the 150 anniversary of the Stroud General Hospital, Gloucestershire Health and Care NHS...

Armed Forces Week and Day 2025
This week we are celebrating Armed Forces Week, and will be marking Armed Forces Day this Saturday (28 June) – a national event to honour the Armed Forces community.

National Healthcare Estates and Facilities Day
Wednesday 18 June is National Healthcare Estates and Facilities Day – a time to recognise the role of the E&F workforce, reflect on the vital work carried out by these professionals, and the value this gives to our patients and colleagues.

Infant Mental Health Awareness Week 2025
Today marks the start of Infant Mental Health Awareness Week (9-15 June). Organised each June by the Parent Infant Foundation, this year’s theme is: Who is holding the baby?

This week is Diabetes Week
Today marks the start of Diabetes Week (9-15 June) – an annual campaign which aims to raise awareness about the things that matter to people with diabetes, and shine a light on what it’s like to live with the condition, day in, day out.

Dietitians Week 2025
Dietitians Week (2-6 June) highlights the important work of registered dietitians across the UK.

Carers Week 2025
Carers Week (9-15 June) is an annual campaign to raise awareness of caring, highlight the challenges unpaid carers face, and recognise the contribution they make to families and communities throughout the UK.

Celebrating our Trust Volunteers
This week is Volunteers' Week, a national event that runs from 2-8 June. It’s a chance to...

Community blood pressure and health checks
Our Community Outreach Vaccination and Health team, together with our One Gloucestershire health and care partners, are supporting the Blood Pressure UK campaign, ‘Know Your Numbers’, all year round, in a bid to reduce heart attacks and stroke.

Heart Failure Awareness Week 2025
This week is Heart Failure Awareness Week (5-11 May). Held every year in May, #HFAW is an opportunity for us to shine a light on heart failure and raise awareness about our fantastic Heart Failure Service.

Council of Governors – nominations now open
Nominations are now open to join our Trust’s Council of Governors. Elections are to be held for the following positions:

New Non-Executive Director Vicci appointed to Trust Board
We are pleased to announce Vicci Livingstone-Thompson has been appointed as a Non-Executive Director to the Trust Board.
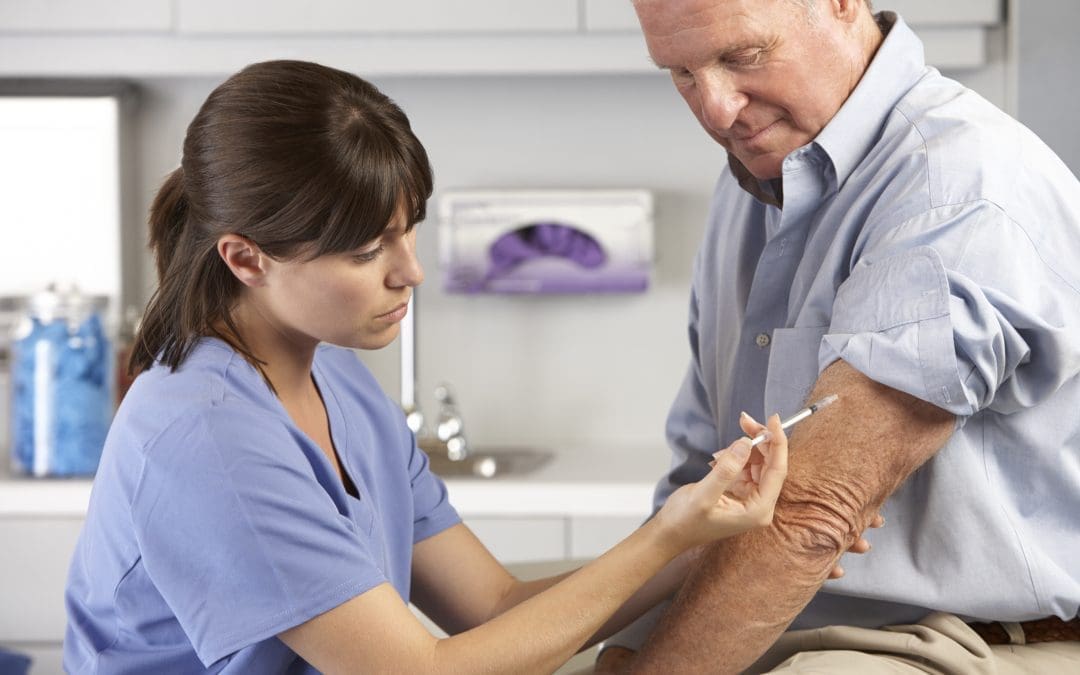
Covid-19 community vaccination clinics
Our Outreach Vaccination and Health Team are offering community COVID-19 drop-in clinics to over 75s and those who are eligible.

Gloucestershire Health and Wellbeing College summer courses
Gloucestershire Health and Wellbeing College is inviting people to sign up for its summer 2025 courses and workshops for physical and mental health.

Better Care Together Awards 2025
Our Better Care Together awards were held at Hatherley Manor Hotel, near Gloucester, today (Weds 9...

Community Mental Health Survey 2025
In August, the NHS is launching a major survey on people’s experiences of using mental health...

Community Mental Health Transformation Newsletter – March 2025
Work on transforming mental health community services in Gloucestershire continues, with a large...

Macmillan Next Steps’ podcast number two now live!
Our team at Macmillan Next Steps has recorded the second in its new series of podcasts.

NHS Staff Survey 2024 results indicate healthy Trust
The 2024 Staff Survey results have been published, providing a detailed annual view of the Trust...

Nutrition and Hydration Week 2025
Nutrition and Hydration Week (17-23 March) is an annual campaign which focuses on the links between our health and what we eat and drink. Our Trust’s theme for this year’s campaign is ‘Bone Health’.
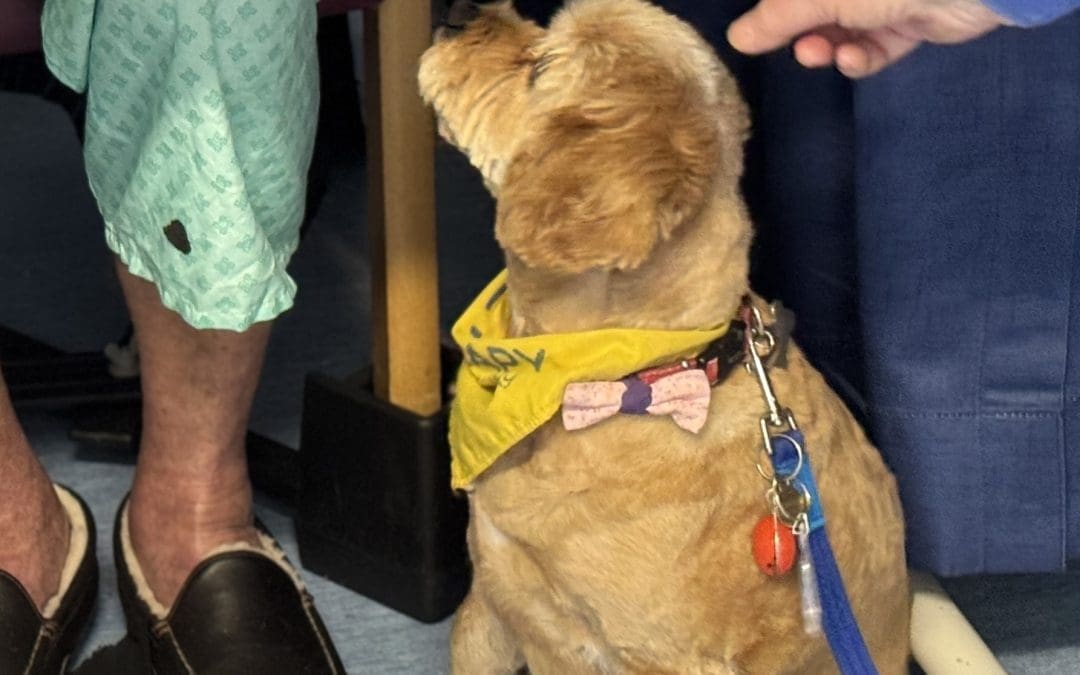
Pets As Therapy at Cirencester Hospital
Pets As Therapy (PAT) is a national charity that aims to enhance the health and wellbeing of...

Apprenticeship Awards – the winners!
A key part of National Apprenticeship Week, our annual GHC Apprenticeship Week Awards provide us...

GHC Charity Update
Our Charity helps to fund additional resources, enhanced patient care and improved therapeutic...

National HIV Testing Week 2025
Today marks the start of National HIV Testing Week (10-16 February). Every year this annual campaign, run by HIV Prevention England, aims to raise awareness about the importance of regular testing, to help reduce the number of people living with undiagnosed HIV and those diagnosed late.

Routine and catch-up HPV jabs for young people aged 12 to 25
The NHS is offering the HPV vaccination to all young people in Gloucestershire from Year 8 to age 25 who have not already received it.
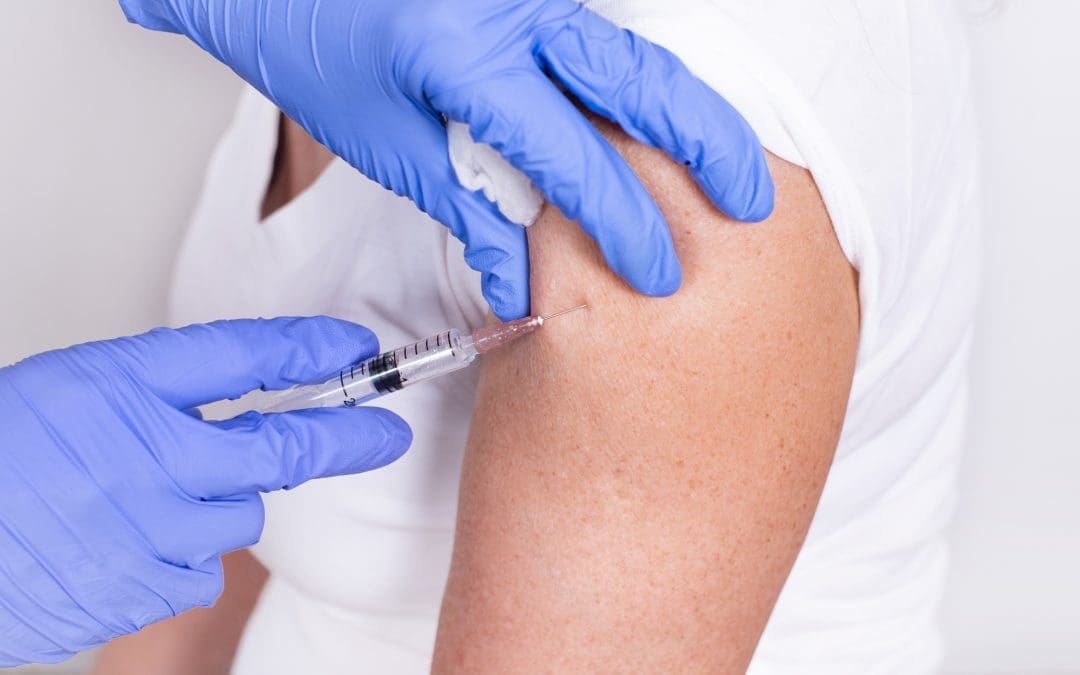
HPV and school-based vaccination community clinics
Our School Aged Immunisation team is currently delivering the human papillomavirus (HPV) immunisation programme in Gloucestershire schools to all children in Year 8, and students in Years 9, 10 and 11 who have not previously taken up the offer.

Macmillan Next Steps launches first in podcast series
Our team at Macmillan Next Steps has recorded the first in what will be a new series of podcasts. In episode one, ‘Returning to Work After Cancer’, Macmillan Next Steps’ Katie Clive talks with Lisa about the physical and psychological challenges she faced when returning to work following her cancer diagnosis and treatment.

Help stop the spread of winter bugs!
Nobody wants to start the New Year with flu, a tummy bug or diarrhoea. However, if you do get poorly, there are a few simple things you can do to help prevent the spread of nasty bugs and viruses.

Vicci recognised in King’s New Year Honours List
Congratulations to Associate Non-Executive Director Vicci Livingstone-Thompson, who has been recognised in the King’s New Year Honours List.

Patient and Carer Race Equality Framework (PCREF) – Update
Work is continuing in our Trust to introduce an anti-racism framework to ensure patients and...

Council of Governors – Election
Nominations are now open for you to join our Council of Governors. Our Council needs the following...

Fair Play campaign launched to tackle gender-based violence
To coincide with this year’s 16 Days of Activism (25 November – 10 December), Hope House SARC (Sexual Assault Referral Centre) and GDASS (Gloucestershire Domestic Abuse Support Service) has launched a new joint campaign called Fair Play.

Notice of Election – Council of Governors December 2024
The Trust gives notice that it will hold elections to the Council of Governors of the...

World AIDS Day – 1st December
Sunday 1 December is #WorldAIDSDay – a global campaign by the National AIDS Trust which has been recognised every year since 1988. Every 1st December communities come together to support and secure the rights of those living with HIV, remember those who have lost their lives to AIDS-related illness, and continue the fight to end the stigma surrounding HIV.

16 Days of Action 2024
16 Days of Action commences on Monday 25 November – International Day for the Elimination of Violence against Women – and runs until Tuesday 10 December, Human Rights Day.

STOP the Pressure Week 2024
This week (18-22 November) is #STOPthePressure Week – a national and worldwide campaign by clinicians to raise everybody’s awareness of pressure ulcer prevention and management.

World Diabetes Day
Today (Thursday 14 November) is World Diabetes Day. This year’s theme ‘Breaking Barriers, Bridging Gaps’, underpins a worldwide commitment to reducing the risk of diabetes and ensuring all people who are diagnosed with the condition have access to equitable, comprehensive, affordable and quality treatment and care.

Minor Injury and Illness Units – Triage Line Update
The triage line to access advice and book appointments at our Minor Injury and Illness Units will...

Colleagues lay wreath as part of Poppies to Paddington initiative
To mark Remembrance Day (11 November), Great Western Railway organised its annual Poppies to Paddington initiative, which transports wreaths from towns and cities across its network to be laid at the war memorial on Platform 1 at Paddington Station, London.

Better Care Together Awards – Get your Nominations in Now!
Nominations are now open for our Better Care Together awards! We will be holding an awards...

Long Service Celebrated at Awards
The long service of colleagues who have worked in the NHS for 20, 30, 40 and even 50 years was...

Occupational Therapy Week 2024
Next Monday (4 November) marks the start of Occupational Therapy Week – an opportunity to celebrate and highlight the role occupational therapy has in people’s recovery and management of their health conditions.

Allied Health Professions (AHPs) Day
Monday 14 October is Allied Health Professions (AHPs) Day. AHPs Day takes place every year in October. The day provides an opportunity to recognise the exceptional contribution our AHPs make to our health and care system, and to raise awareness of the 14 different professions and the varied career paths they offer.

Japanese delegates given tour of community hospitals
Tewkesbury and North Cotswolds community hospitals hosted a special visit from three international delegates yesterday (9 October). The guests, representing the Association of Community Hospitals (ACH) for Japan, were here on a ‘fact-finding’ trip.

Trust hosts its annual AHP Community of Practice Forum
Ahead of next Monday’s National Allied Health Professions’ (AHPs’) Day, our Trust held its second annual AHP Community of Practice Forum on Tuesday (8 October) at Dowty Sports and Social Club in Down Hatherley, Gloucester.

New Associate Non-Executive Director for Trust
A new Associate Non-Executive Director has been appointed to the Board of Gloucestershire Health...

Work for us: Our Mental Health First Point of Contact Centre has expanded
Our First Point of Contact Centre (FPCC) has been evolving to support the national requirement to...

Regional Award for Gloucestershire Mental Health Team
The NHS in the South West is today (5 September) celebrating the remarkable achievements of staff...
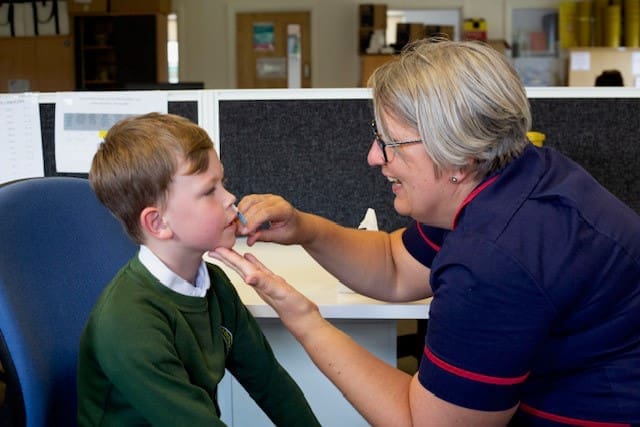
Parents urged to protect their children against flu this autumn
As we enter the 2024-2025 flu season, the School Aged Immunisation team at Gloucestershire Health and Care NHS Foundation Trust is reminding parents and carers of the importance of protecting their children against the virus by ensuring they have their flu vaccination.

Tackling Phobias
Did you know that our Talking Therapies service can treat a range of mental health problems,...
Know your Numbers Week: 2-8 September
The NHS in Gloucestershire is supporting Know Your Numbers Week, an annual campaign led by charity Blood Pressure UK, with a series of health check drop-in events where people can get their blood pressure checked.

Social Worker Shortlisted for National Award
An adult social worker based at Charlton Lane Hospital has been shortlisted in the annual Social...
West Cheltenham Pregnancy Support
If you live in West Cheltenham and are expecting a baby you can meet your midwifery, heath...

Health and Wellbeing College – Autumn/Winter 2024 prospectus
Gloucestershire Health and Wellbeing College (GHW College) delivers educational courses teaching people the skills, techniques and knowledge to make them experts in their own recovery from long-term physical and mental health conditions.

Community Mental Health Transformation Newsletter – August 2024
Since we shared our last update in March, there has been further progress on the Community Mental...

Recruitment for new Integrated Urgent Care Service
Gloucestershire Health and Care NHS Foundation Trust and our partner IC24 are now recruiting GPs...

Annual General Meeting 2024
Our Annual General Meeting will be held on Thursday 19 September 2024 from 5.00 until 6.30pm,...

Stroud Hospitals League of Friends Summer Ice Cream Event
Stroud Hospitals League of Friends hosted its annual Summer Ice Cream Event last Thursday (1 August), as a thank you to staff and volunteers.

Water Damage at Fairford Hospital
Significant water damage at Fairford Hospital means some clinical appointments will need to be...

New Director of Improvement and Partnership appointed
We are delighted to confirm the appointment of Rosanna James as our new Director of Improvement...

Students bring a splash of colour to Cirencester Hospital
The day room on Coln Ward at Cirencester Hospital was the place to be last Thursday (18 July), as dozens of staff and students gathered for the official unveiling of its fabulous new murals.

New Chief Operating Officer for Trust
We are pleased to confirm the appointment of Sarah Branton as our new Chief Operating Officer....

Service users feel positive benefits of gardening
The therapeutic benefits of gardening have been on offer in the Forest of Dean thanks to the...

Update on Sales of Former Lydney and Dilke Hospitals
The opening of the new Forest of Dean Community Hospital means the former hospitals, Lydney and...

‘Hug in a Mug’ initiative on BBC Radio Gloucestershire
The Wellbeing Line is the Gloucestershire Staff Mental Health and Wellbeing Hub, offering confidential mental health and wellbeing support to anyone working in health and social care in Gloucestershire.

Health Checks for People with Serious Mental Illnesses (SMI)
If you are aged 18 or over and have been diagnosed with a serious mental illness such as bipolar...

Trust awarded Veteran Aware reaccreditation
We are delighted to announce that Gloucestershire Health and Care NHSFT has been reaccredited as a Veteran Aware Trust.

Exercise Medical Endeavour 2024
Exercise Medical Endeavour (formerly the South West NHS Military Challenge) took place at Okehampton Army Training Camp in Devon at the weekend (7-9 June).

Time to Talk – Men’s Health Week 10 -16 June 2024
Men’s Health week aims to encourage men to talk, share their stories and access services,...

Princess Royal Officially Opens Hospital
Her Royal Highness the Princess Royal has performed the official opening of the Forest of Dean...
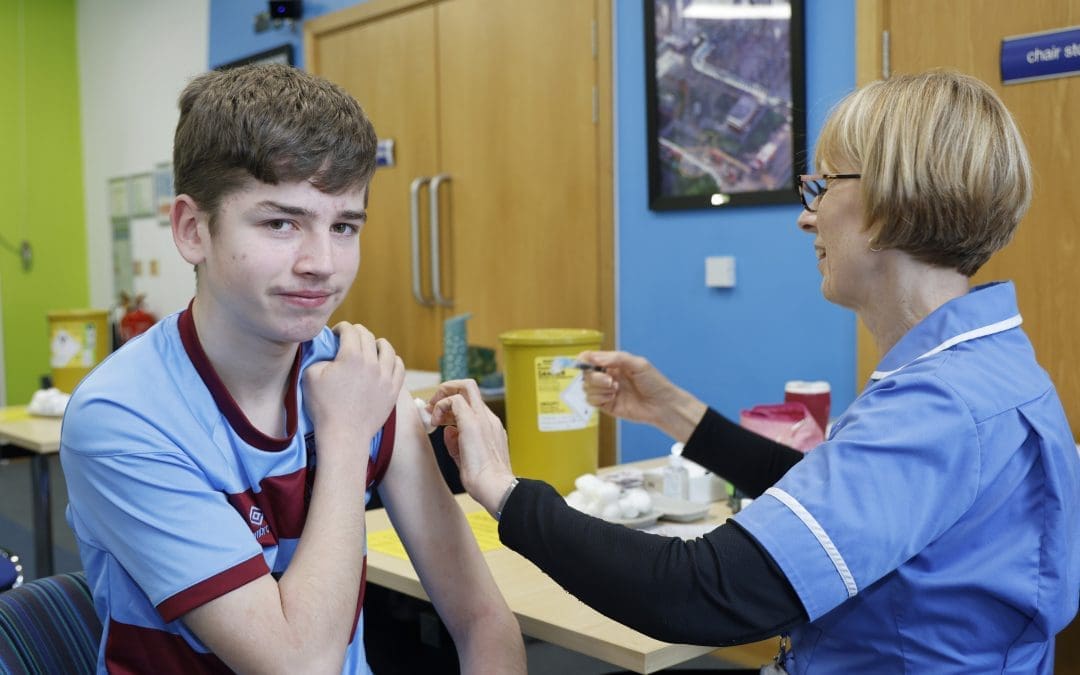
New Electronic Consent Form for School-Age Immunisations
The School Age Immunisation Service (SAIS) is introducing a new way for parents and carers to consent to their children’s school-age vaccinations.

New Non-Executive Directors for Trust
Two new Non-Executive Directors have been appointed to the Board of Gloucestershire Health and...
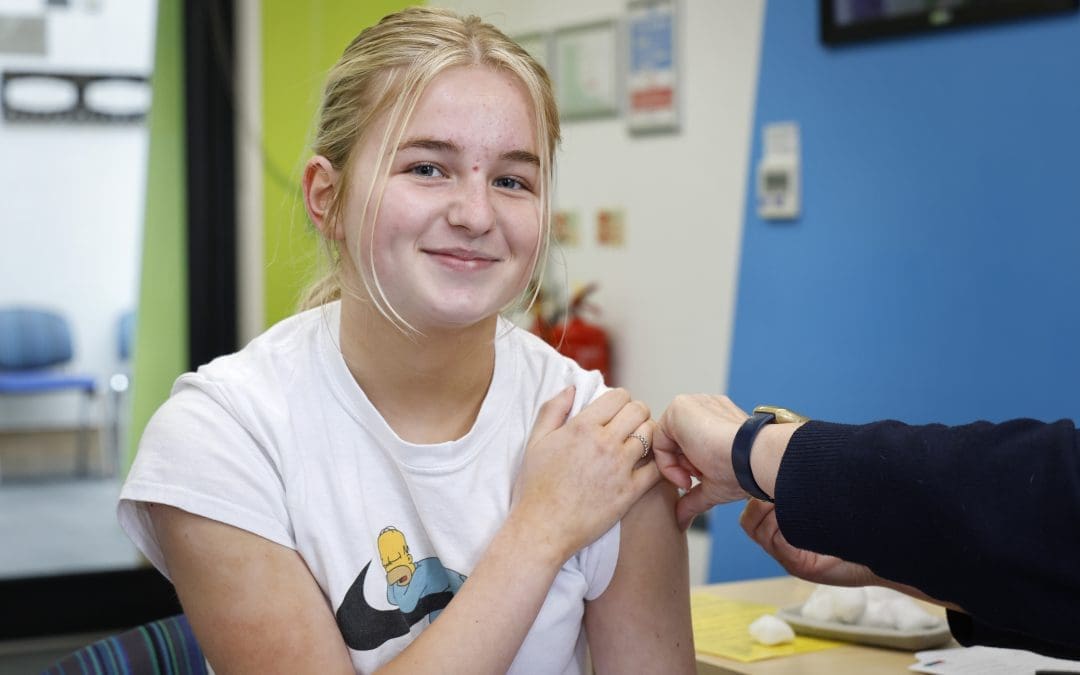
Trust to continue delivery of national immunisation programme
Our School Age Immunisation Service (SAIS) is delighted to be continuing delivery of the national school-based immunisation programme in Gloucestershire.

Integrated Urgent Care Service for Gloucestershire
NHS Gloucestershire has today announced that Gloucestershire Health and Care NHS Foundation Trust...

Mental Health Awareness Week – the power of moving
This week (13-19 May) is Mental Health Awareness Week. Since 2001, the Mental Health Foundation has been leading #MHAW to unite the UK in achieving good mental health.

Forest of Dean MIIU – Update on Service Move
Our Minor Injury and Illness Unit at Lydney Hospital remains open. However, the service will move...

International Nurses’ Day 2024
International Nurses' Day is celebrated around the world on 12 May - the anniversary of Florence...

Ben’s marathon fundraiser for Beat
Ben Gibson was admitted to Gloucestershire Child and Adolescent Mental Health Service (CAMHS) in October 2022, following a clinical diagnosis of depression.

Community Mental Health Survey 2024
We want to know what mental health care is like for young people. You may be sent a letter...

New Director of Nursing, Therapies and Quality for Trust
Following a national recruitment campaign, we have appointed Nicola Hazle as our new Director of...

Farewell Celebration for Trust Chair, Ingrid
Colleagues, former colleagues, partners, volunteers, Experts by Experience and family members...

Dementia Action Week – May 13-19
Colleagues will be out and about across Gloucestershire in May helping people to understand how to...

Using Cognitive Behavioural Therapy to Manage Stress
Not feeling like yourself right now? Maybe you’re feeling irritable, worried, scared, struggling...

Community Mental Health Transformation Newsletter – March 2024
Since we shared our last update in January, there has been further progress on the Community...

Grants Totalling £300k For Projects to Support Mental Health
The Community Mental Health Transformation (CMHT) programme, led by Gloucestershire Health and...

Twiddle mitts bring a splash of colour to Windrush Ward
Patients and colleagues at Cirencester Hospital were thrilled and very grateful to receive these fabulous twiddle mitts from talented knitter Margaret in Bradley Stoke, Bristol.

Countryfile star opens ‘fantastic’ new cabin and workshop
Our therapeutic allotment at Montpellier received a special visit on Friday from farmer and BBC TV presenter Adam Henson, who dropped in to officially open the site’s newly-constructed cabin and workshop.

A look back at Nutrition and Hydration Week 2024
Last week was Nutrition and Hydration Week (11-17 March) – an annual campaign which focuses on the links between our health and what we eat and drink.

New Chair Selected for Trust
A new Chair has been selected for Gloucestershire Health and Care NHS Foundation Trust. Graham...

Today is International Long COVID Awareness Day
Today (15 March) is International Long COVID Awareness Day. Now in its second year, the campaign aims to raise awareness of the symptoms of Long COVID, and the NHS support available to those suffering from the condition.

Celebrating Tewkesbury CATU Anniversary
Our Community Assessment and Treatment Unit (CATU) held a Tea Party on Monday (11 March) to mark...

Positive workplace picture from Staff Survey results
Our Trust's Staff Survey results were released yesterday, reflecting the positive outlook of...

Better Care Together Awards – The Winners!
More than 135 colleagues gathered to celebrate our Better Care Together awards at Hatherley Manor...

Campaign launched to drive up childhood vaccinations
The UK Health Security Agency (UKHSA) has today launched a campaign across England to remind parents and carers of the importance of making sure their children are vaccinated against serious diseases – some of which, such as measles and whooping cough, are re-emerging in the UK.

Physiotherapy in the Forest: Helping local residents to regain their confidence
GHC Musculoskeletal (MSK) Physiotherapists Tomas Bullock and Cerys Watcyns are based in the Forest...

State-of-the-art cataract microscope at Tewkesbury Hospital
The countywide Ophthalmology Cataract Service is provided in partnership by Gloucestershire...

Use of Meta Pixel on our website
It has been brought to our attention that the Trust, along with a number of other NHS and other...

A look back at National Apprenticeship Week 2024
Last week was National Apprenticeship Week 2024. The Apprenticeship and Widening Participation team hosted a packed programme of events throughout the week reflecting this year’s theme, Skills for Life.

Mental Health Courses to Restart
Gloucestershire Talking Therapies is restarting face-to-face courses. The courses are aimed at...

It’s National Apprenticeship Week!
It’s National Apprenticeship Week (5-11 February). The theme for #NAW2024 is Skills for Life, which reflects on how apprenticeships can help individuals develop the skills and knowledge they need for a rewarding career, and how employers can develop a talented workforce equipped with future-ready skills.

New Film Encourages Health Checks
A new film has been produced to encourage people with serious mental illnesses (SMI) to access...
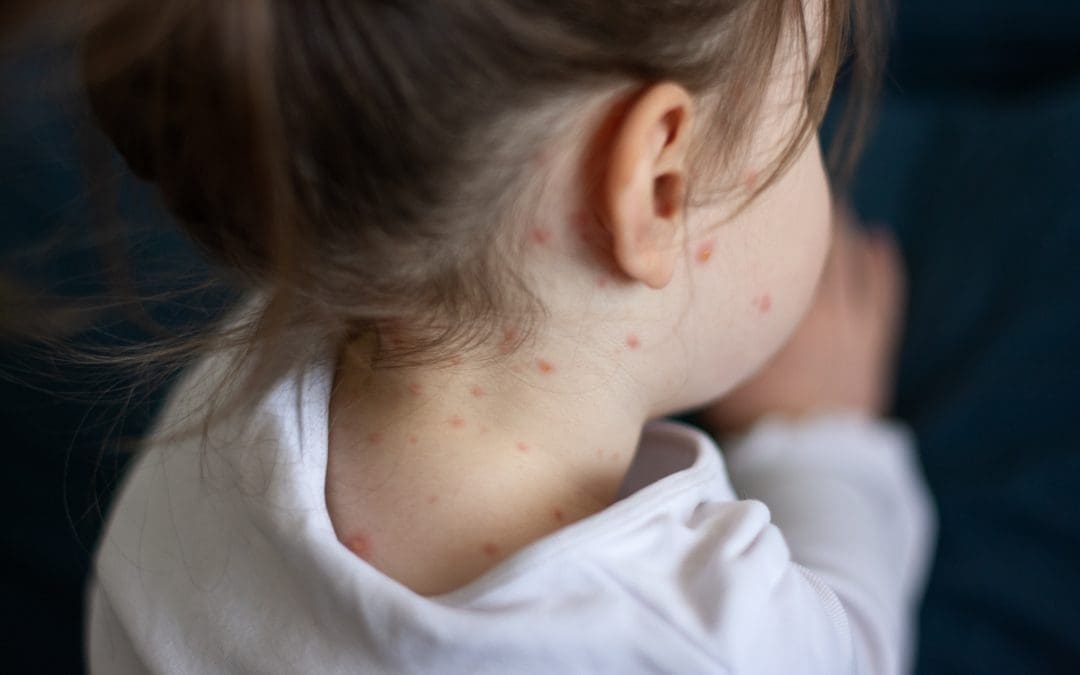
Measles: Parents urged to ensure their children are protected
With the number of reported measles cases in young people in the UK on the rise, the School Age Immunisation Team at Gloucestershire Health and Care NHS Foundation Trust is urging parents and guardians of children in Years 8 to 11 (aged 12 to 16) to check their MMR status and make sure they are fully vaccinated against the disease.

Not Been Feeling Like Yourself Lately?
According to recent research, nearly half* of those living in the South West felt concerned about...

Farm visitors bring a ‘Good Day’ to Charlton Lane Hospital
Last week, Charlton Lane Hospital in Cheltenham received a special visit from residents of The Good Day Farm in Chipping Campden – a mobile farm which brings its animals to the community.

Community Mental Health Grants – Second Opportunity to Apply
A new round of grants are being made available to Voluntary, Community and Social Enterprise...

NHS expands mental health support for veterans
The NHS is rolling out an expanded mental health support service for Armed Forces veterans, as a...

Community Mental Health Transformation Newsletter – Edition 5
Since we shared our last update in September, there has been further progress on the Community...

Industrial Action – Changes to Services in Gloucestershire
Members of the British Medical Association - Junior Doctors - will take industrial action from...

Seven New Queen’s Nurses for Trust
Colleagues from our Trust have been given the prestigious title of Queen’s Nurse (QN) by community...

Ward Sister Lou wins award for dementia tool
Congratulations to Ward Sister Lucinda (Lou) Williams on scooping the ‘Seeing Me Award’ at this year’s South West Integrated Personalised Care Awards. Lou, who specialises in dementia care, was celebrating with her colleagues on Abbey View Ward at Tewkesbury Community Hospital this morning, after picking up the award at last night’s glittering ceremony at Darlington Hall in Totnes, Devon.

Occupational Therapist Neil Scoops National Award
Congratulations to Occupational Therapist Neil Withnell, who was crowned Housing Occupational...

Sign up as an NHS Cadet
NHS Cadets is a programme created by St John Ambulance in partnership with the NHS. It’s designed...

Trust presented with Defence ERS Gold Award
Representatives from Gloucestershire Health and Care NHS Foundation Trust were extremely proud and honoured this morning to receive the Defence Employer Recognition Scheme (ERS) Gold Award from the Wessex Reserve Forces’ and Cadets’ Association (WRFCA), in recognition of its commitment and support for defence personnel.

Charlton Lane Hospital enjoys a flying visit!
Charlton Lane Hospital in Cheltenham recently enjoyed a flying visit from Gerald, Henry and Wally...

Plaque Unveiled in Honour of District Nursing Founder
Professional Head of Community Nursing, Nancy Farr, was invited to unveil a plaque in honour of...

Introducing the Patient and Carer Race Equality Framework (PCREF)
We are working with NHS England to implement the first ever anti-racism framework for mental health Trusts and service providers. The Patient and Carer Race Equality Framework (PCREF) will ensure that we are responsible for co-producing and implementing concrete actions to reduce racial inequality within our services, with a view to becoming an actively anti-racist organisation.

Recruitment Underway for New Chair
Recruitment is underway to find a new Chair for Gloucestershire Health and Care NHS Foundation...

Recruitment for New Director of Nursing, Therapies and Quality
Following the recent announcement that our Director of Nursing, Therapies and Quality John...

Forest of Dean Hospital Update
The new Forest of Dean Community Hospital is due to open in Spring 2024 and we have recently...

Pastoral Care Quality Award for Trust
We’re delighted to have received the NHS Pastoral Care Quality Award for the high level of care...

Gloucestershire Health & Wellbeing College courses – 2023
Our Gloucestershire Health & Wellbeing College (formerly the Recovery College and Glos Self...

Falls Awareness Week 2023
Join our Falls Education Services at events across the county, starting on Monday 18 September,...
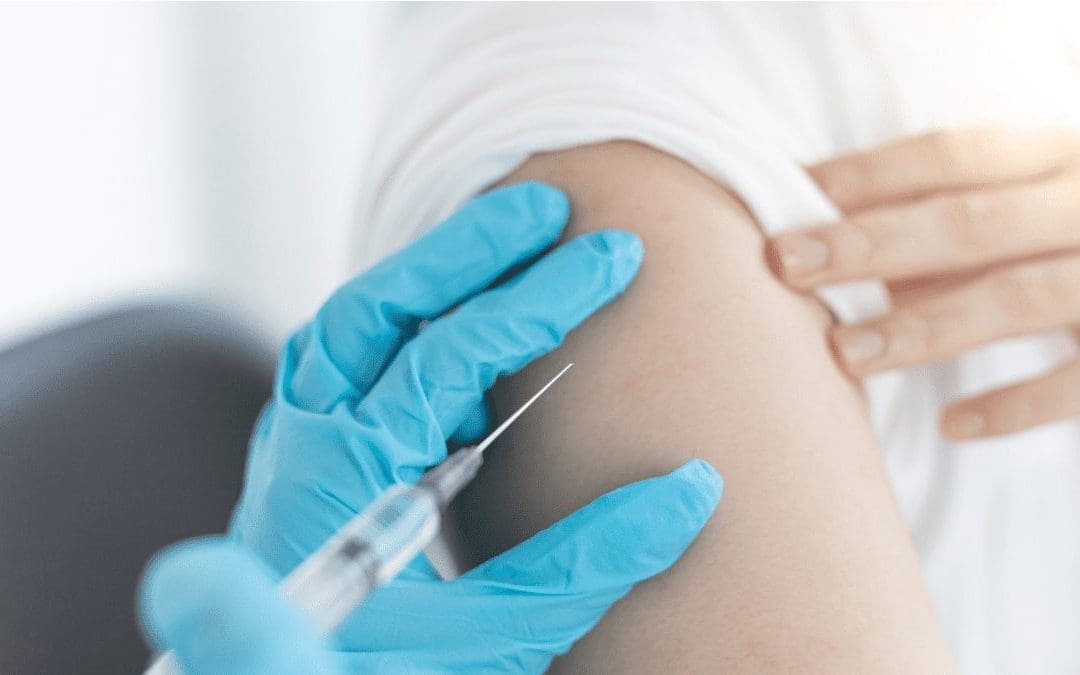
HPV vaccination programme moves to single dose
The Human papillomavirus (HPV) vaccine helps to prevent HPV-related cancers from developing in boys and girls. While most types of HPV are harmless, some high-risk types can lead to the development of cancers, including cervical cancer, cancers of the head and neck (mouth and throat) and cancers of the anus and genital areas.

Sexual Health Week: 11-17 September
Today marks the start of Sexual Health Week. Being safe means feeling empowered to access contraception, testing and treatment. It means understanding consent, healthy relationships and pleasure. It also means providing relationships and sex education (RSE) that gives young people the tools to navigate the world safely – both online and offline – and delivering safe, accessible sexual health services, wherever people need them. That’s why for #SHW23 we’re #PlayingItSafe!

Community Mental Health Transformation: Small Grants
As part of the national programme of Community Mental Health Transformation, we are introducing a...

Mental Health Act Managers
We're looking for a number of Mental Health Act Managers, who have a unique and very important...

Supporting those in need of emergency mental health support in Gloucestershire
You may have heard of a new initiative called Right Care, Right Person, which may change the way...

DIALOG training for VCSE Organisations
Training is being offered to people working in voluntary, community and social enterprise (VCSE)...

Falls Prevention Awareness Week: September 18-22
Gloucestershire Health and Care NHS Foundation Trust is committed to empowering all older adults in Gloucestershire to reduce their risk of falls, which are one of the greatest causes of serious injuries and death among people over age 65. On September 18-22, GHC is partnering with the National Council on Aging (NCOA) to mark Falls Prevention Awareness Week.

Community project shortlisted for HSJ award
A joint NHS community project in Gloucestershire to tackle health inequalities has been...

New Mental Health Training Dates
Free training is being offered to voluntary, community and social enterprise (VCSE) partners...

Veterans Moving Forwards recovery course
The autumn programme of recovery course Veterans Moving Forwards starts next month. The course has been co-produced with veterans and is offered by Gloucestershire Health and Wellbeing College.

Community Mental Health Survey 2023
We believe providing high quality mental health care for everyone is fundamentally important....

Results Day Support for Students
Our Apprenticeships and Widening Access Team are offering support for those getting their results...

World Breastfeeding Week: 1-7 August
World Breastfeeding Week officially kicks off tomorrow, each year celebrated around the world from 1-7 August. Gloucestershire Health and Care NHS Foundation Trust’s Health Visiting team offers a range of support, including advice on positioning, attachment, hand expressing and assisting you and your family to continue to breastfeed for as long as planned. If problems occur, your health visitor can refer you to our Specialist Breast Feeding team.

Hope House sexual health community clinics reopen
Hope House is pleased to announce its face-to-face community clinics are up and running again. Due to Covid-19 our clinics at Coleford Health Centre, Stroud, Cirencester and Tewkesbury community hospitals, Hartpury University, Hartpury College and the Royal Agricultural College, have been restricted to telephone and video consultations only.

New sensory room at Evergreen House officially opened
A new sensory room has been opened at Evergreen House in Cheltenham, thanks to the generosity of a local children’s charity.

International Self-Care Day – 24 July 2023
The World Health Organisation's Self-care Month ends Monday 24 July with International Self-Care...

Community Nurses Medical Bags
Community Nurses are feeling the benefit after the Trust invested in new medical bags to organise...

Community Mental Health Transformation Newsletter – Edition 4
Since we shared our last update in May, we've made even more progress on the Community Mental...

Quality Mark for Preceptorship Programme
We are proud to announce that we have been awarded the National Preceptorship Interim Quality Mark...

Trust Support for Veterans Achieves Gold Award
We are proud to have achieved the Gold Employer Recognition Scheme Award for our work to support...

Public Governor Elections – Nominations Open Now
Nominations are now open for six Public Governor positions in the following areas: Public:...

Trust named Large Employer of the Year in the SW Apprenticeship Awards
Gloucestershire Health and Care (GHC) is celebrating the news that it has been named Large...

Cervical Screening Awareness Week: 19-24 June
This week (19-24) June is Cervical Screening Awareness Week – a campaign launched in 2021 to encourage those eligible for screening to respond to their cervical screening invitation letters and book an appointment at their GP practice or sexual health clinic if they missed their last one.

Allotment team celebrates national awards success
The Montpellier Allotment Project Team celebrated success at the national Design in Mental Health Community Awards when they received a ‘Highly Commended’ in the Outside Space of the Year category.

Mental Health Awareness Training
Free training is being offered to voluntary, community and social enterprise (VCSE) partners...

Community Mental Health Transformation Newsletter – Edition 3
It's Mental Health Awareness Week so the perfect time for us to share another update on Community...

Mental Health Engagement Events
Booking is now open for a series of engagement events to learn more about Community Mental Health...

Dealing with Anxiety
Mike Dexter is a Senior Psychological Wellbeing Practitioner with NHS Talking Therapies,...

Community Mental Health – Survey 2023
Our trust will soon be carrying out a survey to understand what you think about your care. This is...

CAMHS text messaging
As part of our work to reduce missed appointments and ensure that only those who need our service...

Surprise retirement celebration for CEO Paul
Colleagues past and present gathered at Churchdown Community Centre yesterday (Thursday 30 March) to throw a surprise farewell celebration for our Trust’s CEO Paul Roberts, who is set to retire in April.

Better Care Together Awards 2023
Our Better Care Together awards took place this afternoon (23 March) at Kingsholm Stadium, in...

Community Mental Health Transformation Newsletter – Edition 2
There's been a lot happening since we sent our last newsletter out in January. This includes a...

CaSA – Charlton Lane’s carers support group
CaSA (Care and Support Always) is a monthly support group for carers of patients of Charlton Lane Hospital (whether current or recently discharged).

Trust celebrates 2022 Staff Survey results
Our Trust is delighted with its positive and encouraging results from the NHS Staff Survey...

Allotment team offer battery hens a new home – and lease on life!
Members of the Montpellier Allotment Project Working Party embarked on an...

High Sheriff takes in progress on new Forest Hospital
The High Sherriff of Gloucestershire and Vice Lord Lieutenant of Gloucestershire were the latest...

New Associate Non-Executive Director for Board
A new Associate Non-Executive Director has been appointed to the Trust’s Board. Vicci...

Congratulations to our 2023 Apprenticeship Awards winners!
In celebration of National Apprenticeship Week (6-12 February), the Apprenticeship and Widening...

Community Mental Health Transformation Newsletter – edition 1
Community Mental Health Transformation (CMHT) is underway in Gloucestershire, with the Forest of...

King Street move for Physio and Podiatry
Stroud’s Podiatry and Adult Physiotherapy services have moved into the new £6.5m medical centre...

Royal Visit to Newly Developed Therapeutic Allotment
Her Royal Highness The Princess Royal visited our newly developed therapeutic allotment in...

Veteran Support Boosted by Step into Health
The support we give to serving military personnel, veterans and military families is set to be...

Our Carers’ Charter
Our Carers’ Charter was developed with, and for, carers as a joint statement of how we will work...

Special hospital visitors Pringle and Widget spread a little festive cheer!
Penguins Pringle and Widget have been delighting staff and patients at two of our community...

Industrial Action – 15 December 2022
In response to the planned industrial action announced by the Royal College of Nursing (RCN), the...

Arts Psychotherapies
'Arts Psychotherapies' is an umbrella term for the four professions working psychologically and...

New Chief Executive for Trust
A new Chief Executive Officer has been appointed to Gloucestershire Health and Care NHS Foundation...

Oliver McGowan Mandatory Training launches in England
The long-awaited rollout of the Oliver McGowan Mandatory Training in Learning Disability and...

Sustainability
The Trust's Sustainability Strategy has just been published, laying out our approach for the next...

World Occupational Therapy Day
World OT Day was first launched on 27 October 2010 by the World Federation of Occupational Therapists (WFOT). Since then it has become an important date in the occupational therapy calendar to promote and celebrate the profession internationally.

Montpellier allotment redevelopment project
For years the Montpellier allotment and green space at Horton Road, Gloucester, has provided an...

Lord-Lieutenant presents Trust with Defence ERS Silver Award
Lord-Lieutenant of Gloucestershire, Mr Edward Gillespie OBE DL, presents veteran and GHC's Lead...

Access scheme for aspiring clinical psychologists from under-represented backgrounds
As part of our ongoing commitment to addressing issues of diversity and inclusion within the...

Ward refurbishment work underway at Cirencester Hospital
Work to improve the patient experience as well as fire safety on the wards at Cirencester Hospital has recently started. Our Trust is upgrading the fire compartmentalisation on both Windrush and Coln Wards…

Apprenticeship Award Success for GHC
Gloucestershire Health and Care NHS Foundation Trust was named Employer of the Year for the second...

Community Mental Health Transformation in Gloucestershire
The NHS Long Term Plan and NHS Mental Health Implementation Plan 2019/20 – 2023/24 set out that...

CQC Congratulates Trust on ‘Very Good’ Report
The NHS Trust providing community physical, mental health and learning disability services for...

Stroud Hospital refurbishment completed
Following an extensive £2m building project Gloucestershire Health and Care NHS Foundation Trust...

NHS rainbow badges and lanyards
NHS rainbow badges and lanyards You may have spotted some of our staff wearing NHS rainbow badges...

New Anti-Social Behaviour Pledge for Gloucestershire
A pledge has been signed by Gloucestershire leaders, promising that anti-social behaviour will be taken seriously, made easier to report and tackled in partnership.

New Non-Executive Director Appointed to Trust Board
A new Non-Executive Director called Nicola de Longh has been appointed to the Board of Gloucestershire Health and Care NHS Foundation Trust.

Ground Breaking Marks Official Start of Forest Hospital Build
A ground breaking ceremony has been held to mark the official start of building a new community hospital in the Forest of Dean.

Oliver McGowan: NDTi publishes final evaluation report
During 2021, Gloucestershire Health and Care NHS Foundation Trust formed one of four national...

Healthcare Support Worker Week celebrated across the Trust
Our healthcare support colleagues are a critical part of our workforce. Put simply, we could not...

Trust celebrates Armed Forces Week with Defence ERS Silver Award
This week (20-26 June) we're celebrating Armed Forces Week and Armed Forces Day (Saturday 25...

Paul Roberts Announces Plan to Retire
Paul Roberts has taken the decision to retire as our Chief Executive at the end of March 2023. He...

Parliamentary Award for Eating Disorders Lead Sam
A clinician from Gloucestershire Health and Care NHS Foundation Trust has won The Lifetime...
Wotton Lawn Hospital: A great place to work
Wotton Lawn Hospital is an 88-bed acute mental health hospital located in the heart of Gloucester....

Our Experts by Experience
Experts by Experience are people who have personal knowledge of our services, either through their...

End of Life Property Bags for Dying Matters Week
If you know your feed-dogs from your bobbin, your tacking from your frogging, then the Trust would...

Working with the Prince’s Trust to recruit new talent
Our Apprenticeship and Widening Access Team are delighted to be involved with the One...

Easter Health advice and Pharmacy Opening Times
Plan ahead for a healthy and happy Easter The NHS in Gloucestershire is urging people to keep...

Community diabetes service receives ‘gold standard’ seal of approval
Our Community Diabetes Service is celebrating the news that its patient education programme has...

Local artists create mural for launch of On Your Mind Glos
Local artists have used street art to mark the launch of On Your Mind Glos and to help raise...

Volunteers add 175 trees to Cirencester hospital grounds
Many thanks to the friendly people at Moore Allen & Innocent who are at Cirencester Hospital today (Thursday 3 Feb) to add some life to the grounds.

Team of the Week – Wotton Lawn Hospital
Our Team of the Week is Wotton Lawn Hospital in Gloucester! Wotton Lawn Hospital is a mental...

Air conditioning among upgrades at Cirencester Hospital
A series of upgrades have been carried out at Cirencester Hospital through 2021. Coln and Windrush...

Plans for £65k allotment project outlined
For years the Montpellier allotment and green space at Horton Road, Gloucester, has provided an...

Raising awareness of birth-related trauma
Colleagues at Gloucestershire Health and Care NHS Foundation Trust and midwives from...

Better Care Together Awards Celebrate Success
Our annual Better Care Together awards took place virtually - to celebrate the dedication and...
Police and Crime Commissioner visits Hope House SARC
Hope House SARC received a virtual visit yesterday (Friday 26 November) from Gloucestershire's...

World Mental Health Day – 10 October
World Mental Health Day is led annually by the World Health Organisation, and is aimed at raising awareness of mental health issues.

Team of the Week: Integrated Community Teams
Our *team of the week* is our Integrated Community Teams (ICTs) who bring together community...

International Nurses Welcomed to Trust
An international recruitment drive has led to 40 new nurses joining our Trust. The nurses, who are...

Stroke Unit at Vale highly commended by Community Hospital Association
Vale Hospital in Dursley has been highly commended by the Community Hospitals Association (CHA)...

Team of the Week: Recovery Team
Our Team of the Week is our amazing Recovery Team They provide a comprehensive community...

Tewkesbury Hospital receives award for Covid response
A brilliant collective response at Tewksbury Hospital to the Covid pandemic has been formally...

Team of the Week: Mental Health Intermediate Care Team (MHICT)
This week our Team of the Week is Reablement and Home First. The reablement teams are part of the...

We’re celebrating 10 years of our ESD team
The Stroke Early Supported Discharge Team (ESD) was set up 10 years ago in 2011 to enable people...
Better Care Together – New Strategy Launched by Trust
A new five-year strategy has been officially launched by the NHS Trust which provides community...

Join Our Team: Estates Team
Find out more about Estates Team, including current job opportunities available within the team.

HRH The Princess Royal Visits Trust
HRH The Princess Royal has spoken to colleagues from our Trust about their work throughout the...

Administrative Professionals Day: Jovelyn Masters
Jovelyn Masters, Personal Assistant to Associate Director of Patient Safety and Learning, talks about her experience of working at GHC.

Administrative Professionals Day: Jon Allard
As part of our celebration of Administrative Professionals Day, Jon Allard, ICT Business and Project Lead, talks about his experience of working at GHC.

Administrative Professionals Day: Evie England, Apprentice Learning and Development Administrator
Evie England, Apprentice Learning and Development Administrator, shares her professional experience in celebration of Administrative Professionals Day.

10 Common Myths About Apprenticeships That Aren’t True
As part of National Apprenticeships Week 2021, the Apprenticeships team have gathered together some interesting myth-busting facts about apprenticeships and what it’s like to be an apprentice.

Be Well Gloucestershire: Improving access to support in the county
A new campaign is being launched to encourage people across Gloucestershire to ‘Be Well’ and...

Winter Lockdown: Looking After Your Mental Wellbeing
As we head into a second national lockdown in England, we’ve put together ten top tips that be of use when looking after your mental wellbeing over the next month.

Managing infection control in mental health settings throughout a pandemic
Louise Forrister details the challenges of managing infection control in mental health settings throughout a pandemic.

Men and Mental Health in BAME Communities
I was recently asked to write this blog about men in the ‘Black, Asian & Minority Ethnic'...

Views of Children and Young People to Help Shape Local Mental Health Services
Children and young people, parents, carers and health and social care professionals in...

Coronavirus Update
The NHS in Gloucestershire and Public Health England (PHE) are well prepared for outbreaks of new...

Trust Signs Armed Forces Corporate Covenant
Gloucestershire Health and Care NHS Foundation Trust (GHC) has affirmed its support to the armed...

Melanie Triumphs at Apprenticeship Awards
Senior Community Health Care Support Worker Melanie Woodman has been crowned Healthcare Apprentice...

Forest of Dean Community Hospital Citizens' Jury
Following the decision of Gloucestershire Care Services NHS Trust and NHS...

Sarah’s Story – PTSD
As part of Mental Health Awareness Week, we are sharing stories of how people have benefited from...

Digital Therapy Now Available Through Let’s Talk
If you’re experiencing stress, anxiety, depression or similar issues, there’s now a new way of...

Find out about Macmillan Next Steps on BBC Radio Gloucestershire
Listen to Clare Lait, Specialist Community Physiotherapist, talk about the...

#Handitback: Help us to help others by returning your equipment
In Gloucestershire we have a campaign to get any equipment with a GIS Barcode that is unused...

New Eating Disorders Support Group
New Eating Disorders Support Group

